- Khetsiwe P Masuku
- PhD (University of Pretoria), MPH (MEDUNSA); BCommunication Pathology (University of Pretoria)
- Lecturer, University of the Witwatersrand
- Khetsiwe.
This email address is being protected from spambots. You need JavaScript enabled to view it.
- Juan Bornman
- PhD (University of Pretoria); M (Communication Pathology) (University of Pretoria); BLogopaedica (University of Pretoria)
- Professor, Centre for Augmentative and Alternative Communication, University of Pretoria
-
This email address is being protected from spambots. You need JavaScript enabled to view it.
- Ensa Johnson
- PhD (University of Pretoria), MA (University of Pretoria), BA Hons (University of Pretoria), BPrim Ed (University of Pretoria)
- Senior lecturer, Centre for Augmentative and Alternative Communication, University of Pretoria
-
This email address is being protected from spambots. You need JavaScript enabled to view it.
- KP Masuku, J Bornman & E Johnson ‘Access to healthcare for persons with disabilities in Eswatini: A triadic exploration of barriers’ (2021) 9 African Disability Rights Yearbook 138-159
- http://doi.org/10.29053/2413-7138/2021/v9a7
- Download article in PDF
Summary
Eswatini ratified the United Nations Convention on the Rights of Persons with Disabilities (CRPD) and its Optional Protocol in 2012, subsequently developing the National Disability Policy. Regardless of this ratification and the best intentions of the National Disability Policy, healthcare disparities still exist between persons with and without disabilities. This study aims to describe the barriers experienced by persons with disabilities when accessing healthcare services by focussing on the accounts of persons with disabilities themselves, caregivers of persons with disabilities and healthcare professionals. A further aim was to propose recommendations to address these identified barriers. A qualitative case study approach utilising focus groups was employed. Participants for the three focus groups were purposively selected. Data was analysed using a framework approach, employing Nvivo 1.5 qualitative analysis software. Findings revealed that access to healthcare for persons with disabilities was a challenge in Eswatini due to the unavailability of resources in the form of rehabilitation healthcare practitioners and assistive devices; lack of reasonable accommodation especially for persons with visual and communication impairments; stigma and discrimination; transportation costs as a result of the distance of healthcare services; and the lack of social support grants. Recommendations from this study propose an urgent need for Eswatini to be deliberate in implementing initiatives such as disability conscientisation programmes to address stigma and discrimination and to create an awareness of especially communication and visual disabilities. Intersectoral involvement, community engagement projects as well as addressing policy gaps are essential if Eswatini intends to mitigate these barriers.
1 Introduction
Persons with disabilities account for approximately 15 per cent of the global population with almost 80 per cent of all persons with disabilities living in low-and-middle income countries (LMICs).1 In Eswatini the prevalence of disability is 16 per cent.2 Women constitute the majority of persons with disabilities in Eswatini as they make up 58 per cent of the population of persons with disabilities. In total, 82 per cent of persons with disabilities in Eswatini reside in rural areas. Despite having the same healthcare needs as persons without disabilities, persons with disabilities may require additional healthcare as a result of their impairments or the consequences of their impairments.3 However, access to healthcare continues to be a challenge for this population.4 As a result, persons with disabilities experience unmet healthcare needs.5 LMICs such as Eswatini account for the majority of persons with disabilities who experience unmet healthcare needs.6 These unmet healthcare needs are further compounded in persons with disabilities who reside in rural areas, engulfed by poverty and who have limited access to information, education and healthcare.7
Access to healthcare is a broad and complex phenomenon with no single generally acceptable definition.8 Hence it is unsurprising that various scholars interpret access to healthcare differently. It could be argued that the interpretation of access to healthcare is also influenced by context. For the purpose of this study, access to healthcare is defined using Peters et al’s four dimensions framework, as it was developed within the LMIC context. In Peters et al’s 9 framework it is proposed that access to healthcare is the judicious use of amenities according to the needs of the individual and that access encompasses four dimensions, namely availability, acceptability, financial accessibility and geographical accessibility. Peters et al10 further emphasise that quality of care is a fundamental element of each of the four dimensions of their framework.
2 Evolution of healthcare rights through human rights frameworks
Access to basic healthcare is an essential and non-progressive human right that every living human being should enjoy throughout their lifespan, regardless of race, gender, religion, political beliefs, economic and social conditions.11 This declaration by the World Health Organisation therefore creates a legal obligation for global, regional and national structures to ensure that the right to healthcare for everyone - most importantly those who have been previously excluded from such services - is protected and upheld. It was thus inevitable that the focus on access as a human rights’ issue would be actioned through the development of copious global policies and conventions. For example, in the eighties, the United Nations12 through the Standard Rules on the Equalisation of Opportunities for Persons with Disabilities declared that disability should be approached from a human rights perspective. Subsequently, access to healthcare for all African citizens is advocated for and emphasised in several articles of the African Charter on Human and People’s Rights on the Rights of Persons with Disabilities.13 Articles 15 and 16 of the Draft Protocol of the African Charter on Human and People’s Rights14 provide for access to healthcare and rehabilitation for persons with disabilities. It is also declared in the draft protocol of the African Charter on Human and People’s Rights that, every person with a disability has the right to healthcare and it further mandates states to ensure that appropriate and effective measures are put in place to ensure that persons with disabilities have access to these services on an equal basis with others.15
The development of the Convention of the Rights of Persons with Disabilities (CRPD) in 200616 was a momentous landmark in the recognition of human rights for persons with disabilities globally. The CRPD is arguably the most important international human rights’ document ever ratified on behalf of persons with disabilities.17 This is partly because the CRPD outlines and delineates the complete array of human rights that apply to all human beings and centres them in the context of the core existence of persons with disabilities.18 The purpose of the CRPD is to ‘promote, protect and ensure the full enjoyment of all human rights and fundamental freedoms by persons with disabilities and to further promote respect for their inherent dignity’.19 Articles 25 and 26 pertain to the rights of access to health and rehabilitation for persons with disabilities respectively.20
3 Healthcare rights framework in Eswatini
Eswatini ratified the CRPD and its Optional Protocol in 2012.21 To enforce the CRPD, Eswatini developed the National Disability Policy of Eswatini in 2013.22 Subsequently, the National Disability Bill of Rights and the National Disability Plan of Action were developed in 2014 and 2015 respectively.23 It is important to mention that to date, the National Disability Bill of Rights is yet to be passed as law which has direct implications for the implementation of the National Disability Policy.24
Access to healthcare for persons with disabilities is specifically addressed in sections 4.9 and 4.10 of Eswatini’s National Disability Policy.25 In an analysis of the National Disability Policy,26 it was established that the policy document had promised access to healthcare to persons with disabilities at primary, secondary and tertiary levels of care. A detailed analysis and findings on the policy analysis is described in Masuku et al.27 In particular, the policy is committed to ensure the availability of free comprehensive healthcare, assistive devices, rehabilitation and counselling by qualified healthcare personnel at all levels of state healthcare to persons with disabilities and their families, with reference to affordable healthcare in private healthcare facilities.28 In the National Disability Policy, specific emphasis was placed on the availability of sexual and reproductive health services for persons with disabilities because historically persons with disabilities in Eswatini have not had access to information and accessibility to services which would enable them to make informed decisions on their sexuality and reproductive health.29 Community awareness and community mobilisation regarding health promotion to prevent disabilities was further promised in the National Disability Policy. Acceptability was also pledged in the National Disability Policy through advocating for accommodating persons with disabilities such as making alternative communication methods such as sign language available, providing health information in accessible formats and ensuring physical access, for example, wheelchair ramps to buildings.
Prior to Eswatini’s ratification of the CRPD, the protection of the rights of every citizen of the country was committed to in the Constitution of the Kingdom of Eswatini.30 Section 30 of the Constitution particularly focuses on the upholding of the rights of persons with disabilities. Moreover, in section 60 the provision of basic healthcare for every citizen of the country was committed to.31 Although Eswatini’s Constitution does not necessarily make specific reference to access to healthcare for persons with disabilities, it does, however, commit to establishing laws that will ensure that persons with disabilities live productive and meaningful lives in Eswatini.32
There is evidence to suggest that globally, there are compliance challenges with the mandates of the CRPD as domestic laws and policies developed and implemented by signatory states in an attempt of domesticating the CRPD, are often not transferred into practice. Ultimately, the vision of the CRPD for persons with disabilities is currently not fulfilled in Eswatini. This challenge is not unique to Eswatini, as other LMICs such as South Africa33 and Malawi34 are also struggling with achieving access to healthcare for persons with disabilities. There has been a call for global research targeted towards the CRPD implementation process in LMICs.35 The results of the lack of implementation of disability legal frameworks in LMICs are observed in healthcare challenges. Therefore, despite the ratification of the CRPD, healthcare accessibility remains a challenge for persons with disabilities in Eswatini. To our knowledge, the experiences of persons with disabilities when accessing healthcare services in Eswatini from their own perspective, have not been previously explored. As such, it is important to determine how persons with disabilities, caregivers of persons with disabilities and healthcare professionals experience the access to healthcare for people with disabilities in Eswatini in order to create a triadic understanding of the barriers faced by persons with disabilities.
4 Methods
Consistent with the aim of determining the experiences of persons with disabilities when they access healthcare services in Eswatini, a qualitative case study research design was employed.36 Three focus groups comprising of participants from a range of backgrounds and with varied experiences of disability - specifically in relation to healthcare - were utilised. Focus groups were deemed appropriate to achieve the aim as it encourages engagement, explanations and reasoning about the subject at hand. In this case, access to healthcare for persons with disability, bringing both agreements and differences to the fore.37 The current study was approved by the Research Ethics Committee of the Faculty of Humanities, University of Pretoria (reference GW20160721HS). The research team comprised of the first author and a MSc student (research fieldworker) who had training in qualitative methods and has experience of living and working in Eswatini.
4.1 Participants
Participants were eligible to participate in the study if they were 18 years and older, were either persons with disabilities, caregivers of persons with disabilities or healthcare professionals who had knowledge and/or experience with healthcare access for persons with disabilities. Participants were purposively recruited from three different groups, namely persons with disabilities, caregivers of persons with disabilities and healthcare professionals to allow for a diversity of views (Table 1). Moreover, these diverse groups were purposely selected as it was believed that their experiences, understanding and interpretation of access to healthcare for persons with disabilities may differ. In total, 25 participants (15 females and 10 males) with a mean age of 40.6 years (range 30-50 years) were recruited to participate in one of the three focus groups (see Table 1). The first focus group comprised of five persons with disabilities; the second group comprised of six caregivers of persons with disabilities who cared for and accompanied persons with disabilities to healthcare facilities; and the third group of 14 healthcare professionals who treated persons with disabilities on a day to day basis at healthcare facilities. In order to accommodate the large number of healthcare professionals, two separate, but similar focus groups were conducted. The research team which conducted the focus groups were not acquainted with any of the participants.
4.2 Recruitment
After ethics approval and permission from the relevant authorities were obtained, persons with disabilities and caregivers of persons with disabilities were recruited using the data base of the national disability organisation and healthcare professionals via a public tertiary state hospital. The study information letter which included an invitation for participants to take part in the study, was shared with the president of the national disability organisation as well as the director of health and the superintendent of the hospital. Potential participants then directly contacted the research assistant telephonically to indicate their interest to participate in the study.
4.3 Procedure
The focus groups with persons with disabilities and caregivers of persons with disabilities were conducted at a dedicated space at the Mbabane National Library, while the focus group with healthcare professionals was conducted in the hospital boardroom. The first author acted as the moderator and facilitated each of the focus groups. Each group began with the participants’ completion of a consent form and a demographic questionnaire. Participants were then issued name tags and given an option to use a pseudonym. The moderator welcomed participants and introduced herself and the research fieldworker. Participants were asked to introduce themselves. The researcher gave a detailed background of the study and explained the purpose of the focus groups. The rules of the discussion were outlined and agreed upon by all participants. The researcher used a self-developed focus group script, asking one question at a time. Each participant was afforded an opportunity to respond. The research fieldworker used a project chart to highlight key discussion points. After the discussion of each question, the researcher captured and summarised the main points and asked participants to confirm the correctness of their responses (namely, member checking). After all the questions had been completed and participants agreed that they had nothing further to add, the moderator thanked the participants for their time and constructive participation and the focus groups ended. Transport and lunch stipends were provided to the two groups of participants comprising of persons with disabilities and caregivers of persons with disabilities, while lunch was offered to the healthcare professional participants. A focus group procedural checklist was followed for all groups to ensure procedural reliability. Reliability was checked by the research fieldworker and was found to be 98 per cent across all three focus groups. Each focus group lasted approximately one hour (ranging between 51.43 minutes and 125 minutes). Focus groups were audio-recorded and transcribed verbatim by the first author and checked by the research fieldworker.
4.4 Data analysis
A framework approach to data analysis was employed in this study,38 using NVivo 1.5 qualitative data analysis software to manage the data and to label and explore themes.39 In accordance with the framework approach, the data analysis steps proposed by Gale et al40 were employed to identify, analyse and report on patterns that existed within the data, ultimately described as themes. The first step involved the first author familiarising herself with the data through replaying and re-reading the transcripts to immerse herself in the data. In the second step, the transcripts were subjected to line by line collaborative coding by the first and last author in order to identify patterns in the data. Ultimately a code book was developed. The third step involved searching for themes by combining codes with similar contents. The fourth step entailed refining themes and further dividing them into sub-themes, with excerpts from participants to support the themes. The fifth step involved relabelling themes using short phrases. A theme was accepted if it had several quotes from the data to support it. The final step involved mapping the themes obtained from the data onto the Peters et al41 access to healthcare framework, namely: availability, acceptability, geographical accessibility and financial accessibility.
4.5 Rigour
This study applied the trustworthiness strategies proposed by Shenton,42 namely credibility, transferability, dependability and confirmability. Furthermore, to ensure trustworthiness, triangulation of data from three data sources was used and member checking was done by going through participants’ responses after each question to check for accuracy of reporting. Collaborative coding also ensured credibility as did peer scrutiny via online and onsite PhD forums as well as through a conference presentation where a part of the findings of the study was presented. Trustworthiness was further ensured through providing an in-depth description of the study methodology, which is also available through an audit trail and a detailed reflection journal as well as through representation of a specific inclusion and exclusion criteria facilitated transferability. The three groups recruited from diverse backgrounds ensured that multiple perspectives were obtained.
5 Findings
The findings and discussion of the study are presented according to the four dimensions of the access to healthcare framework as described by Peters et al.43 The specific themes conceptualised under each of the four dimensions are discussed below.
5.1 Availability of healthcare services as a barrier
Two different themes which are related to availability were conceptualised. They are discussed separately.
5.1.1 Availability of assistive devices
In Eswatini, there appears to be inconsistency with the issuing and maintenance of assistive devices. With the lack of a budget dedicated to the procurement and maintenance of assistive devices by state hospitals, persons with disabilities acquired assistive devices from various sources. Assistive devices were received from donations arranged by community members, donations from non-governmental organisations and sometimes from the national health fund (the Phalala fund), as explained by Caregiver #3: ‘I eventually got courage to speak up [at a community meeting] and I got help because they gave me a wheelchair, even though the wheelchair is not in use now’. Healthcare professional #2 stated: ‘[P]ersons with disabilities do receive assistance from the Phalala fund to get prosthetic limbs from South Africa once-off. The challenge comes when the prosthetics need to be repaired’. However, Healthcare Professional #11 painted a bleaker picture: ‘There are no assistive devices and other communication aids’.
5.1.2 Availability of rehabilitation facilities and healthcare professionals
The distribution of healthcare professionals varied across the different healthcare facilities, with the majority of comprehensive healthcare services located in tertiary hospitals. The location of rehabilitation services in referral hospitals presented with access challenges due to the fact that referral hospitals are situated in major cities, far removed from the rural areas where the majority of persons with disabilities reside. Healthcare Professional #6 explained it as follows: ‘Mbabane is probably the only hospital that has all the health services together under one roof, if you would go to hospitals in the periphery, you would find maybe medical and nursing with a physio being the only rehabilitation professional’. Caregiver #4 expressed the same concern: ‘ They [healthcare professionals] say that they have these services, but the problem is that these services are centralised to referral hospitals, yet the people who need these services are [on] the outskirts of town and it’s not easy for them to come through to town’.
Of specific concern was the reported shortage of rehabilitation services due to the general shortage of professionals in this sector as highlighted by Healthcare Professional #11: ‘ There is a limited number of allied professionals especially speech language therapists’. Healthcare Professional #6 attributed this to the fact that rehabilitation posts are not prioritised or budgeted for: ‘ Basically, there is no budget line allocated towards rehab services and this facility has to find a way of making or being able to procure stuff for their department’.
5.2 Acceptability of persons with disabilities in healthcare facilities as a barrier
Only one theme, namely the lack of reasonable accommodation was conceptualised under the construct acceptability.
5.2.1 Lack of reasonable accommodation
Although it appears as if the Department of Healthcare in Eswatini has made significant strides in making physical access to healthcare facilities through the enactment of wheelchair ramps and wider waiting area passages, this was not consistent across all healthcare facilities. Person with Disabilities #3 explains: ‘At the dispensary, there is a step that makes it difficult for [a] person on a wheelchair to get closer to the medicine counter when one wants to collect medication. When I get my medication sometimes, I need to shout for the attention of the person at [the] dispensary window’.
Communication and health information consideration were also lagging behind. As a result, persons with communication and visual difficulties still experience challenges when consulting with healthcare professionals as well as when they attempt to make sense of health information given to them as can be seen in the following statements from 2 respective participants: ‘When you get to the dispensary, sometimes you find that the tablets that are given to you have instructions that are not written in braille’ (Person with Disability #1); and ‘[t]hey just give you the medication without asking and knowing whether you can read or not or whether you understand what is written on the pills or not’ (Person with Disability #2). Healthcare Professional #3 was also aware of this fact: ‘There are no braille signs for the visually impaired to be able to navigate around the facility’.
Futhermore, Healthcare Professional #6 noted similar challenges for deaf persons: ‘There are nurses and some of us here that have been trained in sign language, but the challenge, I am sure my colleagues will agree with me, that you attend the sign language training, but when you come back you do not use it and then lose it’.
Discrimination was the challenge most frequently mentioned by participants across all three groups. Stigma and discrimination seemed to be prevalent within families of persons with disabilities and their communities, mostly as a result of how communities understand disability and its causes. Healthcare professionals could be seen as an extension of the community that still views disability from a negative perspective. Furthermore, some healthcare professionals harbour negative stereotypes which ultimately influence how they treat persons with disabilities in healthcare facilities, as explained by Healthcare Professional #10: ‘Lack of knowledge of all disability conditions amongst us’, and Healthcare Professional #11: ‘Lack of awareness and experience of healthcare workers/professionals with persons with disabilities’.
Participants particularly mentioned self stigma, wherein caregivers of children with disabilities hid their children away from their communities for fear of judgement as evident in the following statement by Caregiver #4: ‘Some of us hide our children with disabilities because we don’t want our communities and community health workers to know about them. They lock the children in the houses’. Caregiver #1 confirmed barriers related to stigma: ‘So, you don’t want people to know that you had the bad luck of having a disability or having a child with a disability so because you don’t want the community to know, you just hide the child’.
Participants also mentioned that persons with disabilities were excluded by healthcare professionals from certain health programmes, especially those related to sexual and reproductive healthcare as mentioned by Caregiver #4 in the following statement: ‘Even if you do get there [hospital], there is now the struggle with attitude. They will ask you “Mummy how many children do you have?” You will say that this is my fourth. They will tell you that the reason why you ended up with a child with a disability is because you kept giving birth’. Person with Disability #5 further confirmed this finding: ‘Yes, the nurse will ask you what you were doing when you fell pregnant. You feel embarrassed because you feel like nothing, like you have committed a sin’.
5.3 Financial accessibility of healthcare services as a barrier
Inconsistency in the allocation of social support grants was the theme conceptualised under financial accessibility.
5.3.1 Inconsistency in allocation of social support grants
Persons with disabilities often depend on social support grants which they normally receive on a monthly basis for their livelihood. In Eswatini, the allocation of social support grants is not a consistent standard procedure as is the case in other LMIC countries. It was reported by participants that some persons with disabilities were receiving social support grants while others did not. In cases where persons with disabilities were receiving these grants, they did not receive the grants consistently. Caregiver #1 explained it as follows: ‘We [persons with disabilities] have been placed under the public assistance [social grant] as a by the way, because it has always been a secret and not everyone has been aware of it. It [social grant] has been a hidden thing and the criteria for receiving is still not clear’.
Apart from the inconsistency of the provision of social grants, there was also a lack of clarity on whether or not healthcare services were free for persons with disabilities despite being promised as such in the National Disability Policy. This was explained by Healthcare Professional #5 in the following statement: ‘Persons with disabilities would not pay for health services, I heard that the ministry would provide free healthcare services’. Healthcare Professional #6 also confirmed this: ‘Free health services for persons with disabilities has not yet been implemented’.
As a result, persons with disabilities experience financial challenges when accessing healthcare as can be seen in the following statements from Caregiver #5 and Healthcare Professional #11: ‘Because we live under difficult financial conditions, we don’t have the money to go up and down to and from the hospital because as a mother I also have other children to look after’ (Caregiver #5); ‘Inaccessibility to public transport, such as having to pay extra for wheelchairs, or paying for the person accompanying the disabled person’ (Healthcare Professional #11).
5.4 Geographical accessibility of healthcare services as a barrier
Transportation needs was the theme conceptualised under geographical accessibility.
5.4.1 Transportation needs
Due to specific impairments experienced by persons with physical disabilities which render them unable to walk to healthcare facilities, the majority of participants reported the need for transportation to access healthcare. Furthermore, participants stated that rehabilitation healthcare services in primary and community healthcare were not easily accessible to them as most were far from their place of residence as reported by Caregiver #5 in the following statement: ‘ You will go to the hospital and after assessing your child, they will tell you to come once or twice a month for review, but because the hospital is far you can’t keep appointments’.
It was also mentioned that outreach services were not available to persons with disabilities. Transportation is costly for persons with physical disabilities because they have to pay transport for themselves and for their caregivers. Furthermore, they have to pay extra for their wheelchairs to be transported. Negative attitudes of public transport drivers unfortunately do not make the process of taking public transportation easier for persons with disabilities and their families. The following statements from Caregiver #5 explain this more clearly: ‘As mothers, these children become heavy and it becomes a challenge to have to carry them on your back. Especially when you have one with cerebral palsy such as mine’; and ‘Because even with the wheelchairs, you have to leave it at home sometimes because it causes a problem on the bus. You have this insensitive bus conductor complaining about your wheelchair’.
6 Discussion
This study aimed to describe the barriers experienced by persons with disabilities when they access healthcare services from a triadic perspective and also aimed to propose recommendations to address these identified barriers. Findings from this study indicate that, despite it having been eight years since the inception of the National Disability Policy of Eswatini, persons with disabilities still experience substantial barriers that hinder them from accessing healthcare services adequately. A large scale study conducted by Eide et al44 in four LMICs, namely Sudan, Namibia, Malawi and South Africa with the aim of identifying the magnitude and impact of specific barriers for persons with disabilities to accessing healthcare, obtained similar findings to those of the current study. Eide et al45 specifically revealed that 10-40 per cent of persons with disabilities do not get to access general healthcare when they need it.
Findings from the study at hand reveal that barriers to accessing healthcare in Eswatini were as a result of the unavailability of healthcare resources - in particular human resources and assistive devices. Human resources, specifically, rehabilitation healthcare professionals such as occupational therapists, speech language therapists, audiologists, physiotherapists and social workers do not have a dedicated budget for their posts. As a result, Eswatini has a limited number of rehabilitation professionals, with the majority of services located in referral hospitals which are in larger towns which are situated far away from rural areas where many persons with disabilities reside - a finding also reported by Bright et al.46 In 2011, the World Health Organisation reported that only a small percentage of persons with disabilities had access to basic rehabilitation services when they needed them, a finding confirmed by the research of Sherry47 and Hussey et al,48 respectively. It is concerning that a decade later similar experiences are still being reported by persons with disabilities. Health rehabilitation is regarded as an important prerequisite for access to all other rights.49 Therefore, the significant contribution of rehabilitation healthcare professionals in addressing and overcoming participation barriers through different interventions which can be focussed on the environment, and on individuals and/or their families, cannot be over emphasised.50
Consistent with findings from studies conducted in similar LMIC contexts such as Malawi, South Africa, Namibia and Sudan by Eide et al;51 Harrison et al;52 and Matter and Eide,53 the findings from the current study also revealed that Eswatini did not have a dedicated budget for the issuing and maintenance of assistive devices. As such, persons with disabilities have no option but to seek assistive devices from community members or from non-governmental organisations. A national fund called ‘Phalala fund’ was mentioned as having been instrumental in assisting with assistive devices. However, it was stated that these assistive devices referred to are devices such as prosthetics which could only be obtained in South Africa. Where devices were obtained through this fund, maintaining them remained a constant challenge due to the lack of a dedicated budget for this purpose.
The accommodation of persons with physical disabilities with the provision of wheelchair ramps and the widening of waiting area spaces - even though this was not the case for all hospitals - was noted in Eswatini. Regrettably, findings revealed that the needs of persons with communication, hearing or visual impairments were not accommodated when accessing healthcare in Eswatini. This could be attributed to the fact that communication disorders, including hearing impairments, are viewed as invisible disabilities.54 In a South African audit, Hanass-Hancock and
Alli55 confirmed these findings where it transpired that half of the facilities in South Africa’s KwaZulu-Natal province had essential features such as ramps, doors and toilets that provided wheelchair access, but almost none provided information in braille or offered sign language interpretation. The lack of reasonable accommodation for these populations, not only impacted on persons with disabilities’ right to access healthcare with autonomy, dignity, privacy and confidentiality, but also had the potential to have life-threatening consequences especially where instructions pertaining to medication were not adequately explained to persons with disabilities in understandable ways. It is not possible to address a person’s right to healthcare without considering the important role of language in fulfilling this right.56 Therefore, it is proposed that healthcare information should be provided in a simplified format and where necessary with visual support or in an auditory format. These findings are echoed in studies conducted by Masuku et al;57 and Orrie and Motsohi.58
With regard to geographical accessibility, there was a general dissatisfaction with the distance of healthcare services in Eswatini, especially the concentration of rehabilitation services in referral hospitals situated in major towns. This finding is supported by Bright et al,59 who revealed that in LMIC’s such as Eswatini, healthcare facilities were mostly situated in urban areas making it difficult and expensive for most people especially those residing in rural areas to access these services. Transportation to healthcare facilities from where persons with disabilities reside, to the facility is thus inevitable. The further the distance is from the healthcare facility, the higher the transportation fare for public transport. As confirmed by Hussey et al,60 the distance to healthcare facilities does impact on persons with disabilities’ financial accessibility of these services. The negative attitudes of public transport drivers towards persons with disabilities further compounded transportation difficulties. In a study titled ‘“You must carry your wheelchair” - Barriers to accessing healthcare in a South African rural area’, the challenges of transportation as they relate to both cost and attitudes was also stressed.61
The fact that, globally, persons with disabilities still do not experience the same access to work opportunities, could lead to a large proportion of them being unemployed.62 With a national unemployment rate of 41 per cent and a poverty rate of 63 per cent in Eswatini,63 the unemployment rate for persons with disabilities in Eswatini is further compounded. This therefore implies a need for social support from the state to support persons with disability financially in their quest to access healthcare services. However, it was found in the current study that there is an inconsistency with the allocation of social support grants in Eswatini, with some persons with disabilities receiving social support and some not. One of the participants mentioned that the social grant: ‘Has always been a secret and not everyone has been aware of it’ (Caregiver #4). Where social support grants were received, they were not on a month-to-month basis. This inconsistency of providing social support grants in Eswatini is contrary to findings from other countries. For example, in South Africa grants are allocated to persons with disabilities to improve their financial situation.64 Although social grants may be offered to persons with disabilities in other countries, it is also important to keep in mind that these grants may not be sufficient, considering that in some cases it may be the only source of income as a result of high unemployment and poverty.65
To conclude this discussion, the South African Human Rights Commission (SAHRC)66 argues that discrimination remains the biggest disability. The statement of the SAHRC also rings true for Eswatini as negative beliefs and stereotypes about the causes of disability continue to perpetuate stigma and discrimination of persons with disabilities when they access healthcare services. Stigma and discrimination are experienced at a personal and a community level as well as at healthcare facilities. Negative attitudes from healthcare professionals, in part because of the lack of knowledge on disability, was confirmed by Eide67 as well as in a study by Hussey et al,68 where all participants cited stigma and negative perceptions towards persons with disabilities in South African society as being the major underlying barrier to health and rehabilitation. Trani et al69 argued that negative stereotypes regarding disability and towards persons with disabilities by healthcare professionals and members of the community, for example public transport providers, stemmed from socialisation and cultural factors resulting in how they treated persons with disabilities. It is therefore important to propose some recommendations to address access for persons with disabilities in Eswatini.
7 Recommendations
Three overarching recommendations are made to address the challenges mentioned in this study.
7.1 Addressing stigma and discrimination
Whether conscious or sub-conscious, stigma and shame are the core catalysts in societies that impede persons with disabilities’ ability to access their rights, including their right to basic healthcare. Stigma and shame regarding disabilities are rooted in the manner in which our cultures and contexts have socialised individuals to perceive disability and ultimately view persons with disabilities and how the community judge what they are capable and incapable of. It tends to manifest itself in the way in which persons with disabilities are viewed and how their value in society is perceived by others. Stigma ranges from the subtle forms of rejection that persons with disabilities experience - sometimes from their own families, such as being hidden from the public eye - to more crude forms of discrimination experienced within communities - such as exclusion from opportunities enjoyed by persons and families without disabilities. As alluded to earlier in this study, healthcare professionals are socialised in holding similar beliefs to those of communities, which results in the perpetuation of stigma and discrimination in healthcare facilities too. Ndlovu70 terms the African view of disability as ‘ambivalent’ in that it depicts disability and persons with disabilities in both a positive and negative light. On the one end, disability is portrayed as burdensome and as a result of an affliction, a punishment, an embodiment of sin, as the works of witchcraft and/or as ancestral anger. While on the other end the African principle of Ubuntu that encapsulates ‘humanness’ dictates that everyone, regardless of social standing should be treated with the dignity that they deserve.71 Initiatives to address access to healthcare for persons with disabilities therefore cannot be done independently of addressing stigma and discrimination.
There is a need for disability conscientisation amongst communities in Eswatini, if attitudes and perceptions about disabilities are to change. Programmes aimed at conscientising communities on disability rights need to be implemented at community level. Communities need to be made aware of the rights of persons with disabilities. At a healthcare level, healthcare practitioners need to be trained on disability rights with specific reference to healthcare rights. Likewise, McConkey et al72 recommend that communities should be educated to understand what causes disability, how to assist persons with disabilities and also highlights that persons without disability should spend time with persons with disabilities, in order for them to realise how similar they are - so called ‘heart knowledge’.
Figure 1 is an example of access to healthcare guidelines that were developed to highlight the core rights to healthcare for persons for disabilities in Eswatini.73 These guidelines were developed for display in healthcare settings to empower persons with disabilities on their right to access healthcare.
Figure 1: Access to healthcare guidelines from Masuku et al74
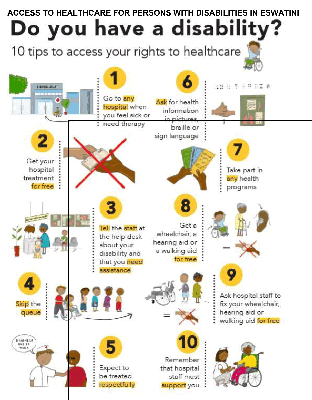
7.2 Intersectoral involvement addressing the social determinents of healthcare
Persons with disabilities are amongst the poorest in most LMIC,75 yet social influences play a significant part in perpetuating poor and decreased quality of healthcare services. Access to healthcare for persons with disabilities across the lifespan is a systemic challenge that is influenced by social determinants of health. It therefore becomes imperative to address social determinants such as access to early life experiences, education, employment, social support, shelter, employment security and community engagement for persons with disabilities76 if healthcare is to be an achievable goal.
Addressing social determinants of healthcare implies the need for an intersectoral involvement as it cannot be the responsibility of the Department of Healthcare or the Department of Social Development alone. For example, to address the geographical and financial accessibility barriers brought about by the location of rehabilitation services in referral hospitals, the government of Eswatini may want to consider a service delivery model whereby such services are brought closer to communities. The principles of community-based rehabilitation propose that persons with disabilities are able to receive healthcare and rehabilitation services within their communities.77 The World Health Organisation defines community based healthcare workers as members of the very same community who are trained by the department of health in this case, rehabilitation healthcare professionals to provide basic rehabilitation techniques. As such, h ealthcare professionals may conduct community and home visits, while at the same time train community based healthcare workers and families on how to conduct basic rehabilitation or how to implement home programmes in between their visits. Strengthening community programmes might mitigate some of the challenges related to geographical and financial accessibility, while at the same time improve attitudes of community members towards disability and persons with disabilities. This strategy has been implemented in certain parts of South Africa in order to address the shortage of healthcare workers. Mulumba et al 78 posit that community participation is not only a human right, but an essential underlying determinant for realising the right to access health.
7.3 Addressing policy shortcomings
It is imperative to determine and communicate the shortcomings of the National Disability Policy of Eswatini in systematic research studies, so that these findings can be considered during the policy evaluation stages. A policy brief was developed to communicate the fact that the policy document has not considered the role of geographical access to services,79 as this is significant in whether persons with disabilities access healthcare or not. The lack of clarity of policy on whether or not the policy was implemented has also been brought to the attention of policy makers. Policy makers have been urged to consider fast tracking the passing of the National Disability Bill of Rights as law. The National Disability Bill of Rights is an integral part of the implementation of the national disability policy. By implementing the bill, the state government of Eswatini would in essence, be committing itself to the realisation of disability rights, including the basic right to healthcare.
8 Conclusion
The right to healthcare is acknowledged in various international and regional human rights instruments and laws. Eswatini being a signatory to most of these human rights instruments, the CRPD in particular, has committed to the realisation of the right to healthcare. Eswatini’s commitment to the right to healthcare was discernible through the development of the National Disability Policy, the National Disability Bill of Rights and the National Disability Plan of Action. Regardless of the development of these local instruments, the right to healthcare for persons with disabilities in Eswatini is yet to be realised as noticeable in the challenges that persons with disabilities still experience when they attempt to access healthcare.
Human rights legislation serves no purpose if states do not commit to implementing these laws. Eswatini needs to recommit to the process of implementation of the National Disability Policy as there is evidence of significant gaps in the process, particularly related to human, skills and financial resources. The passing of the National Disability Bill of Action is key to the process and should thus be prioritised. Policy implementation should be done in the context of social determinants of health.
The implementation of disability legislation should be done parallel to disability conscientisation, starting at community level. Eswatini should therefore be deliberate in adopting programmes aimed at dismantling negative stereotypes regarding disabilities within communities.
2. Deputy Prime Minister’s Office ‘Swaziland National Disability Policy’ (2013) 12; S Mavundla ‘Country report: Swaziland’ (2015) 3 African Disability Rights Yearbook 245 at 247.
3. See generally T Shakespeare et al ‘Access to healthcare for persons with disabilities’ (2018) www.ohchr.org%2Fdocuments%Issues%2FDisability%@FStandardHealth%2F BackgroundDoc_EGM_Righttohealth (accessed 12 November 2020).
4. See generally JAK Harrison et al ‘Access to healthcare for people with disabilities in rural Malawi: What are the barriers?’ (2020) 20 BMC Public Health 833.
6. World Health Organisation ‘Human rights and health’ (2017) https://www.who.int/en/news-room/fact-sheets/detail/human-rights-and-health (accessed 27 December 2021).
7. J Neille & C Penn ‘Beyond physical access: A qualitative analysis into the barriers to policy implementation and service provision experienced by persons with disabilities living in a rural context’ (2015) 15 Rural and Remote Health 3332.
8. See generally B Jacobs et al ‘Addressing access barriers to health services: an alytical framework for selecting appropriate interventions in low-income Asian Countries’ (2012) 27 Health Policy and Planning 288.
9. DH Peters et al ‘Poverty and access to health care in developing countries’ (2008) 1136 Annals of the New York Academy of Sciences 161.
12. UN Department of Economic and Social Affairs ‘Standard rules on the equalisation of opportunities for persons with disabilities’ (1993) https://www.un.org/development/desa/disabilities/standard-rules-on-the-equalization-of-opportunities-for-persons-with-disabilities.html (accessed 27 December 2021).
13. African Union ‘Draft Protocol on the African Charter of Human and People’s Rights’ adopted by the Organisation of African Unity on 27 June 1981, entered into force 21 October 1986.
16. UN General Assembly, Convention on the Rights of Persons with Disabilities (2007) UN Doc A/RES/61/106 (24 January 2007) https://www.un.org/development/desa/disabilities/convention-on-the-rights-of-persons-with-disabilities.html (accessed 27 December 2021).
17. See generally M Perlin ‘International human rights and institutional forensic psychiatry: The core issues’ (2016) American Psychological Association 9.
26. KP Masuku et al ‘Analysing Eswatini’s national disability policy reforms: Access to healthcare implications for citizens with disabilities’ (2020) (accepted).
30. Constitution of the Kingdom of Swaziland, 1996 (as set out in sec 29 (20) of the Citation of Constitutional Law Act 2006)
33. See generally M Hussey, M MacLachlan & G Mji ‘Barriers to the implementation of the health and rehabilitation articles of the United Nations Convention on the Rights of Persons with Disabilities in South Africa’ (2017) 6 International Journal of Health Policy and Management 207.
35. See generally B O’Hare, D Devakumar & S Allen ‘Using international human rights law to improve child health in low income countries: A framework for healthcare professionals’ (2016) 16 BMC International Health and Human Rights 11.
36. K Hammarberg, M Kirkman & S de Lacey ‘Qualitative research methods: When to use them and how to judge them’ (2016) 31 Human Reproduction 498.
38. NK Gale et al ‘Using the framework method for the analysis of qualitative data in multi-disciplinary health research’ (2013) 13 BMC Medical Research Methodology 117.
39. C Brandão ‘P Bazeley & K Jackson Qualitative data analysis with NVivo (2nd ed)’ (2015) 12 Qualitative Research in Psychology 492.
42. AK Shenton ‘Strategies for ensuring trustworthiness in qualitative research projects’ (2004) 22 Education for Information 63 at 73.
44. AH Eide et al ‘Perceived barriers for accessing health services among individuals with disabilities in four African countries’ (2015) 10 Plos One e0125915.
46. T Bright et al ‘A systematic review of strategies to increase access to health services among children in low and middle income countries’ (2017) 17 BMC Health Services Research 252.
47. K Sherry ‘Disability and rehabilitation: Essential considerations for equitable accessible and poverty-reducing healthcare in South Africa’ (2014) 1 South African Health Review.
53. RA Matter & AH Eide ‘Access to assistive technology in two Southern African countries’ (2018) 18 BMC Health Services Research 792.
54. N Tye-Murray Foundations of aural rehabilitation: Children, adults and their family members (2009).
55. J Hanass-Hancock et al ‘“These are not luxuries, it is essential for access to life”: Disability related out-of-pocket costs as a driver of economic vulnerability in South Africa’ (2017) 6 African Journal of Disability 280
56. HJ Haricharan et al ‘Can we talk about the right to healthcare without language? A critique of key international human rights law, drawing on the experiences of a Deaf woman in Cape Town, South Africa’ (2013) 28 Disability and Society 54.
57. KP Masuku, N Moroe & D van der Merwe ‘“The world is not only for hearing people - It’s for all people”: The experiences of women who are deaf or hard of hearing in accessing healthcare services in Johannesburg. South Africa’ (2021) 10 African Journal of Disability 1.
58. S Orrie & TS Motsohi ‘Challenges experienced by healthcare workers in managing patients with hearing impairment at a primary health care setting: A descriptive study’ (2018) 60 Official Journal of the South African Academy of Family Practice/Primary Care 39.
61. R Vergunst et al ‘“You must carry your wheelchair” - Barriers to accessing healthcare in a South African rural area’ (2015) 8 Global Health Action.
62. S Bonaccio et al ‘The participation of people with disabilities in the workplace across the employment cycle: Employer concerns and research evidence’ (2020) 35 Journal of Business and Psychology 135.
69. JF Trani, E Ballard & J Pena ‘Stigma, social exclusion and mental distress of persons with disabilities in Afghanistan’ (2016) 153 Social Science and Medicine 258.
70. HL Ndlovu ‘African beliefs concerning people with disabilities: Implications for theological education’ (2016) 20 Journal of Disability and Religion 29.
72. R McConkey et al ‘Promoting better health for persons with intellectual disabilities through community-based inclusive development’ (2018) Disabilities Innovations Africa Series 6.
74. K Masuku ‘Access to healthcare for persons with disabilities in Eswatini’ PhD thesis, University of Pretoria, 2020.
