- Innocentia Mgijima-Konopi
- Programme Manager Disability Rights Unit, Centre for Human Rights, Faculty of Law, University of Pretoria, Atlantic Fellows for Health Equity South Africa (AFHESA) at Tekano.
- LLB (Hons) (Witwatersrand), LLM (National University of Ireland, Galway)
- The views expressed in this publication are those of the authors and do not necessarily represent those of Tekano, the Atlantic Institute, or their governing boards.
- Mary Auma
- Bachelor of Law (Makerere University, Uganda), LLM (University of Pretoria), LLD candidate (University of Pretoria)
- The authors wish to thank Foluso Adegalu for his editorial assistance
- I Mgijima-Konopi & M Auma ‘Health emergencies post COVID-19: What guidance can Africa’s Disability Protocol provide?’ (2020) 8 African Disability Rights Yearbook 253-263
http://doi.org/10.29053/2413-7138/2020/v7a12 - Download article in PDF
1 Introduction
Several African countries recorded their first cases of the coronavirus disease (COVID-19) in March 2020, the same month the World Health Organisation (WHO) declared it a global pandemic.1 Within three months the virus has spread throughout the continent. By 29 December the Africa Centres for Disease Control and Prevention put the total number of COVID-19 cases in Africa at 2.6 million with 63 300 deaths recorded. 2 Though there are no official statistics on the number of persons with disabilities in Africa who have tested positive for or succumbed to COVID-19, the Working Group on The Rights of Older Persons and People with Disabilities in Africa in its statement on International Day of Persons with Disabilities acknowledged the potential heightened vulnerability of persons with disabilities on the continent to the pandemic reiterating that many persons with disabilities have pre-existing health conditions that may make them more susceptible to contracting the virus and experiencing more severe symptoms, leading to elevated mortality rates. 3
From the start of the pandemic anecdotal evidence emerged that most government’s COVID-19 responses did not fully take into account persons with disabilities. In response, several organisations who work towards combating discrimination against persons with disabilities launched the COVID-19 Disability Rights Monitor (DRM) initiative to collect, analyse and disseminate reliable quantitative and qualitative data on the impact of COVID-19 and related measures adopted by government on persons with disabilities globally.4 Data was collected from respondents from 134 countries through a survey conducted between 20 April and 8 August 2020. A report of the findings, Disability rights during the pandemic: A global report on the findings of the COVID-19 Disability Rights Monitor was launched in October 2020.5 For Africa, the monitoring report helps identify areas where states are failing to take sufficient measures to protect the rights of persons with disabilities in their response to the pandemic.
The discussion that follows focuses on aspects of the monitoring report related to gaps in the protection of right to health of persons with disabilities in Africa during the pandemic.6 The commentary will use the survey results to illustrate how the Protocol to the African Charter on Human and Peoples’ Rights on the Rights of Persons with Disabilities in Africa (African Disability Protocol), once in effect, may provide additional guidance to states in responding more effectively to the health needs of persons with disabilities during possible further ‘surges’ of the COVID-19 pandemic as well as future health care emergencies.7 It concludes with a call for African states to expediently ratify the African Disability Protocol so it can come into force.
2 African regional instruments and the right to health of persons with disabilities during the COVID-19 pandemic
The right to health of persons with disabilities in African states, is well established under different African human rights instruments. The African Charter on Human and Peoples’ Rights (African Charter) provides that every individual shall have the right to enjoy the best attainable state of physical and mental health.8 It further stipulates that ‘the aged and the disabled’ shall have the right to special measures of protection in keeping with their physical or moral needs.9 The African Charter on the Rights and Welfare of the Child guarantees every child the right to enjoy the best attainable state of physical, mental and spiritual health.10 In addition to the these two instruments the Protocol to the African Charter on Human and Peoples’ Rights on the Rights of Women obliges states to ensure that the right to health of women, is respected and promoted.11
Building on these existing regional instruments, the African Disability Protocol makes extensive provision for the protection of the right to health of persons with disabilities. Adopted on 30 January 2018 by the African Union Heads of States,12 the African Disability Protocol is the culmination to date of the African Union’s efforts to create a framework to safeguard the human rights of persons with disabilities on the continent. The potential of the Protocol to contribute to fostering a more inclusive and equitable society in which the human rights of persons with disabilities are respected is yet to be realised. It has not yet attained the 15 ratifications required for it to come into force.13.
Many of the provisions in the African Disability Protocol mirror the provisions of the United Nations Convention on the Rights of Persons with Disabilities (CRPD).14 For instance, using language considerably similar to article 25 of the CRPD, article 17 of the African Disability Protocol guarantees the recognition of the right of every person with a disability to the highest attainable standard of health and requires states parties to take positive steps towards its realisation. There are aspects of article 17 of the Protocol that differ from the CRPD. The African Disability Protocol enjoins states to ensure that ‘health care services are provided using accessible formats and that communication between service providers and persons with disabilities is effective’.15 This obligation is not explicitly set out in the CRPD but rather implied in article 9 on accessibility.16 Similarly, the obligation on states to guarantee that persons with disabilities are provided with support in making healthcare decisions stated in the Protocol is implied under article 12 of the CRPD which deals with equal recognition before the law.17 The Protocol by drawing out these obligations puts emphasis on as well as broadens the understanding of these rights.
Article 17 of the African Disability Protocol also contextualizes the right to health to the African context where many people continue to access healthcare services from informal health care providers.18 It extends the ambit of protection to persons with disabilities accessing informal health services by requiring states to guarantee ‘informal health services do not violate the rights of persons with disabilities’.19 Lastly the Protocol unlike the CRPD speaks to the need for non-stigmatising health campaigns and provision of pain relieving drugs to persons with disabilities which alludes to some of the experiences on the continent.20
3 Identifying gaps in the protection of right to health of persons with disabilities in Africa during the COVID-19 pandemic
3.1 Summary of data collated by the Disability Rights Monitor Research from Africa
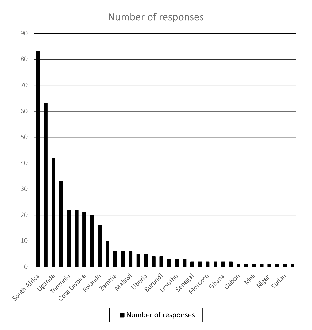
The DRM survey received 397 responses from 34 countries in Africa.21 In terms of regional disaggregation Eastern Africa had the highest number of responses (185), followed by Western Africa (109).22 Figure 1 below shows responses per country. The highest number of responses came from South Africa (83), Nigeria (63) and Uganda (42).
3.2 Composition of the response pool
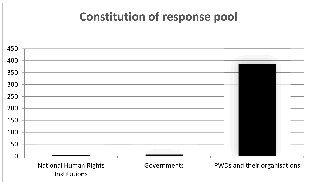
The majority of the responses received as shown in Figure 2 were from persons with disabilities, their families, carers and organisations (386). There were only (7) official responses that came from governments and (4) from national human-rights institutions.
4 Access to medication and essential healthcare services by persons with disabilities in Africa during the COVID-19 pandemic: Survey findings
Though the degree and manner differed, several responses indicated that access to medical-care facilities, services and medication had been severely restricted or limited for persons with disabilities during the pandemic in their countries. This was predominantly linked to a suspension of disability-specific health services in many public hospitals at the onset of the pandemic, inflation and the rising cost of living linked to COVID-19; shortages in medication including psychiatric medication; denial of reasonable accommodation in accessing services and pre-existing poor access to good quality affordable health services in many countries.24 The discussion that follows examines certain of these key findings.
4.1 The impact of rising cost of living on medical care
Respondents from Uganda, Nigeria, Sierra Leone, Zimbabwe, Kenya and Nigeria said that the rising cost of living specifically linked to COVID-19 in their countries meant that many persons with disabilities whose livelihoods were already fragile before the onset of the pandemic could not afford medical care.
In a bid to curtail the spread of COVID-19 governments throughout the region adopted far-reaching measures including the restriction of movement of people and goods, the closure of international borders, lockdowns and curfews.25 These measures have had a substantial adverse impact in many countries on both national economic growth and individual livelihoods.26 For persons with disabilities in Africa the impact of this economic downturn was compounded by the fact that many in this group came into the COVID-19 crisis already experiencing barriers that precluded them from effectively participating in the economic activities of their countries.
As echoed by ILO’s policy brief issued in June 2020, prior to the onset of this crisis a high number of persons with disabilities compared to those without were less likely to be employed or have decent employment conditions, more likely to be in the informal economy and likely not adequately covered by social protection.27 The DRM survey showed that persons with disabilities who earn their livelihoods in the informal sector in particular were badly affected by the disruption in economic activities during the pandemic.28 A respondent from Nigeria pointed out that ‘the increase in the cost of living brought about by COVID-19 has made life very unbearable for persons with disabilities who are self-employed, their families and caregivers’.29
4.2 Access to disability-specific health services during the pandemic
Respondents reported that at the onset of the pandemic disability specific-health services (i.e rehabilitation services and therapies etc.) in a number of their countries’ public hospitals had been suspended to prioritise testing and treatment of COVID-19 patients. One of the respondents from South Africa expressed concern that ‘children with disabilities could not access early intervention programmes as all programmes has been suspended at hospitals and clinics as the government prioritised services to Covid-19 only’. A DPO reported that a number of hospital departments that repair wheelchairs and other assistive devices were closed. While governments prioritised the treatment of COVID-19 patients they failed to ensure that people with disabilities continue to access these crucial services. The impact of this disruption on the health of persons with disabilities affected is yet to be fully understood, but it could lead to mid to-long term worsening of existing conditions and late diagnosis of new impairments.
4.3 Access to medication
The shortages in psychiatric medication in Africa have been well documented, however the advent of the COVID-19 pandemic has made the shortages more acute with medication being out of stock or in short supply in many countries.30 Shortages of medication and related community based mental health services for persons with psychosocial disabilities during the pandemic was a concern for respondents from Uganda, South Africa, Zimbabwe and Kenya. DPO’s from these countries reported that some people with psychosocial disabilities in these countries had stopped taking the medication prescribed to them because they were unable to access it. In other instances, they received different medication to the one prescribed as a substitute. DPO’s expressed fears that these shortages in psychiatric medication may result in deterioration of the mental health of persons with psychosocial disabilities and possible relapses. In countries like Uganda where mental-health services are primarily accessed in psychiatric institutions and not community based, the closure of these institutions during the lockdown left persons who experienced a mental-health crisis during this period without help. The absence of additional measures to mitigate the psychological stress brought about by the pandemic and accompanying measures such as social isolation on both those with pre-existing mental health conditions and without was also mentioned.
4.4 Access to prevention, testing, treatment of COVID-19
With regards to whether persons with disabilities in Africa were able to obtain information about prevention of COVID-19 in accessible formats, personal protective equipment and treatment of COVID-19 on an equal basis with others, 61 per cent of respondents (273) expressed uncertainty as to whether persons with disabilities in their countries had access to COVID treatment on an equal basis with others. Twenty-three respondents were of the view that persons with disabilities were being deprived of treatment, whilst 61 respondents believed that persons with disabilities had equal access to treatment.
Figure 4: Access to COVID-19 treatment
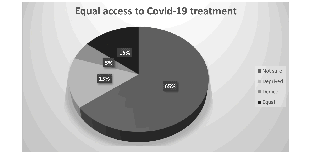
The data from the survey showed that most countries had made a commendable attempt to ensure that persons with disabilities could access information on COVID-19 as well as the countries’ response in accessible formats including sign language and audio formats. A number of respondents however pointed out that information provided was generic and not disability specific. Concern was raised regarding Hospital triage guidelines. Fears arose that the application of triage protocols result in persons with disabilities being disadvantaged from or not prioritised to receive lifesaving resources, such as ventilators, where there are shortages.31
5 How the African Disability Protocol may guide states in protecting the right to health of persons with disabilities in future pandemic
There are a select set of obligations that will arise from the Protocol, once it comes into operation, which could be particularly relevant to the possible further ‘surges’ of the COVID-19 pandemic and future health care emergencies. Firstly, the Protocol recognizes, in the Preamble of article 17 that persons with disabilities have the right to the enjoyment of the highest attainable standard of health. It requires states to ensure persons with disabilities have access to health facilities, goods and services on a non-discriminatory basis.32 Similar to the CRPD discrimination on the basis of disability is defined in article 1 of the Protocol as ‘any distinction, exclusion or restriction on the basis of disability which has the purpose or effect of impairing or nullifying the recognition, enjoyment or exercise, on an equal basis with others.’33 The Protocol in addition also stipulates that the denial of reasonable accommodation itself constitutes discrimination on the basis of disability. 34
In interpreting the right to health in the African Charter, the African Commission on Human and Peoples’ Rights (African Commission) has stressed that the minimum core obligations imposed on a state are to ensure the right of access to health facilities, goods and services on a non-discriminatory basis, especially for vulnerable or marginalised groups.35 The African Commission has stated that states are obliged to ensure that national plans prioritise members of vulnerable and disadvantaged groups in access to healthcare and take steps to ensure that individuals, especially those belonging to vulnerable and disadvantaged groups, are not prevented from accessing healthcare services and goods.36 The African Commission has further reiterated that states are under the obligation to respect the right to health by, inter alia, refraining from denying or limiting equal access for all persons (including persons with disabilities) to health services.37 The African Children’s Committee also echoed a similar opinion as the African Commission in the case of IHRDA and Open Society Justice Initiative (OSJI) (on behalf of children of Nubian descent in Kenya) v Kenya.38
The Protocol therefore once operational reinforces the existing duty of states to prioritise the health needs of persons with disabilities as they constitute a vulnerable group, particularly it could be inferred during health care emergencies where such vulnerability is heightened. Healthcare services including services targeted at addressing those health emergencies ought to be provided on an equal basis without discrimination on the ground of disability. States have a duty of care to provide persons with disabilities with the reasonable accommodation they need in accessing these services. The Protocol places a special emphasis on the importance of providing services using accessible formats.
The Protocol once in force will reinforce the duty of states to provide persons with disabilities with the same range, quality and standard of healthcare as provided to other people. Much like in article 25(a) of the CRPD article 17(2)(a) of the Protocol speaks to states’ obligations to ensure that where the state has systems of free and affordable healthcare people with disabilities should be able to access these on an equal basis with others without discrimination. States therefore must ensure that persons with disabilities do not receive inferior or substandard healthcare compared to fellow citizens during pandemics. Healthcare personnel are required to provide care of the same quality to persons with disabilities as others. Health care policies and practices developed by states during health emergencies to guide healthcare workers on which patients to prioritise to receive life-saving resources, such as admission to the intensive care unit and a ventilator, in the event of shortages may not exclude or disadvantage persons with disabilities on the basis of their disability.
6 Conclusion
The Protocol as highlighted here has the potential once in force to corroborate some key obligation under the right of health in both the CRPD and African Charter amongst others and assist in guiding states to avoid some of the violations witnessed under the current pandemic. Its potential will remain unrealized until African states ratify it.
1. World Health Organisation (WHO) ‘WHO Director-General's opening remarks at the media briefing on COVID-19’ 11 March 2020 https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed 26 November 2020).
3. ‘Statement of the Working Group on the Rights of Older Persons and People with Disabilities in Africa of the African Commission on Human and Peoples’ Rights’, At the Occasion of the International Day of Persons with Disabilities, 3rd December 2020.
4. ‘Covid-19 Disability Rights Monitor’ https://covid-drm.org/ (accessed 21 October 2020).
5. ‘Disability Rights during the pandemic: A global report on the findings of the COVID-19 Disability Rights Monitor’ (Disability Rights Monitor Report) (2020).
6. It is important to note that COVID-19 holds implications for a number of additional rights as well, this commentary is however limited to the right to health.
7. Protocol to the African Charter on Human and Peoples’ Rights on the Rights of Persons with Disabilities in Africa (African Disability Protocol) art 17.
11. Protocol to the African Charter on Human and Peoples’ Rights and on the Rights of Women in Africa, art 14.
13. https://au.int/en/treaties/protocol-african-charter-human-and-peoples-rights-rights-persons-disabilities-africa (accessed 18 December 2020). Nine countries have signed the Protocol at the time of writing, namely Angola, Burkina Faso, Cameroon, Central African Republic, Gabon, Mali, Rwanda, South Africa and Togo.
16. UN Committee on the Rights of Persons with Disabilities, General Comment No 2 (2014), Article 9: Accessibility para 40.
18. M Sudhinaraset, M Ingram, HK Lofthouse & D Montagu ‘What is the role of informal healthcare providers in developing countries? A systematic review.’ (2013) 8 (2) PLoS One.
21. Covid-19 Disability Rights Monitor (n 4). A comprehensive discussion of the methodology of the research falls outside the scope of this commentary but can be found on page 16-21 of the report.
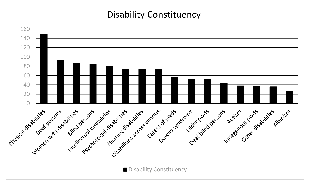
23. The survey allowed for respondents representing organisations to select multiple constituencies where they represented more than one.
25. ‘COVID-19 and the World of Work: Ensuring the inclusion of persons with disabilities at all stages of the response’ (2020) ILO policy brief.
26. ‘Six charts show how COVID-19 is an unprecedented threat to development in Sub-Saharan Africa’ IMF News 13 April 2020 https://www.imf.org/en/News/Articles/2020/04/13/na0413202-six-charts-show-how-covid-19-is-an-unprecedented-threat-to (accessed 15 Nov 2020).
28. ‘COVID-19 Disability Rights Monitor: Irene from Kenya’ https://www.youtube.com/watch?v=11J7Y02fFVA (accessed 17 December 2020) ; ‘COVID-19 Disability Rights Monitor: Sithembile from Eswatini’ https://www.youtube.com/watch?v=0CH0xlc Tv70 (accessed 17 December 2020).
29. The results from the survey show that the strict and indiscriminate enforcement of lockdown and curfew measures, often accompanied by police brutality, also made persons with disabilities and their families afraid and at times unable to leave their homes to access health services and other essential supplies.
30. C Sunkel & M Viljoen ‘Shortage of psychiatric medications in South Africa’ (2017) 4(1) page 15-16. https://doi.org/10.1016/S2215-0366(16)30422-9 (accessed 18 Dec-ember 2020).
31. EL McKinney, V McKinney & L Swartz ‘COVID-19, disability and the context of healthcare triage in South Africa: Notes in a time of pandemic’ (2020) 9 Africa Journal of Disability 2.
34. African Disability Protocol (n 7), art 1 definition of discrimination on the basis of disability.
35. African Commission ‘Principles and guidelines on the implementation of economic, social and cultural rights in the ACHPR’ para 67a.